There are numerous causes of mastitis in cows. It can also be complicated to treat depending on the severity and the source of the infection. Mastitis collectively costs farmers billions of dollars each year in lost cattle.
This common and serious issue that can have a significant impact on animal health, so it pays to learn more about it. This guide explains what mastitis is, how it affects both dairy cows and beef cows, and how best to prevent and treat it.
Table of Contents
What is Cattle Mastitis?
Cattle mastitis can occur in both dairy cattle and beef cattle and is an inflammation of the mammary glands. Intramammary infection can be caused by bacteria, fungi, viruses, and microscopic algae. Chemicals and physical trauma may also be causes of mastitis, though they are less likely.
When mammary glands are infected, cows produce less milk and the quality of that milk significantly declines, and they may cease milk production altogether. Once mastitis is discovered, infected cows must be treated, and milk produced by those cows should be safely discarded.
Mastitis can lead to serious economic loss for farmers and what’s worse, infections can easily spread through the herd. This means that infected cows must be separated from the rest of the herd, and it is pivotal to discover the cause and severity of the infection so it can be promptly dealt with.
Symptoms of Mastitis
There are two main classes of symptoms of mastitis: subclinical and clinical.
Subclinical
In subclinical mastitis cases, it may not be evident that a cow has it because there are few observable symptoms. Farmers may or may not notice a small decrease in the amount of lactation.
Unfortunately, subclinical mastitis is often under-treated due to the lack of outwards signs, even though it has a high prevalence within dairy herds as evidenced by milk testing.
Clinical
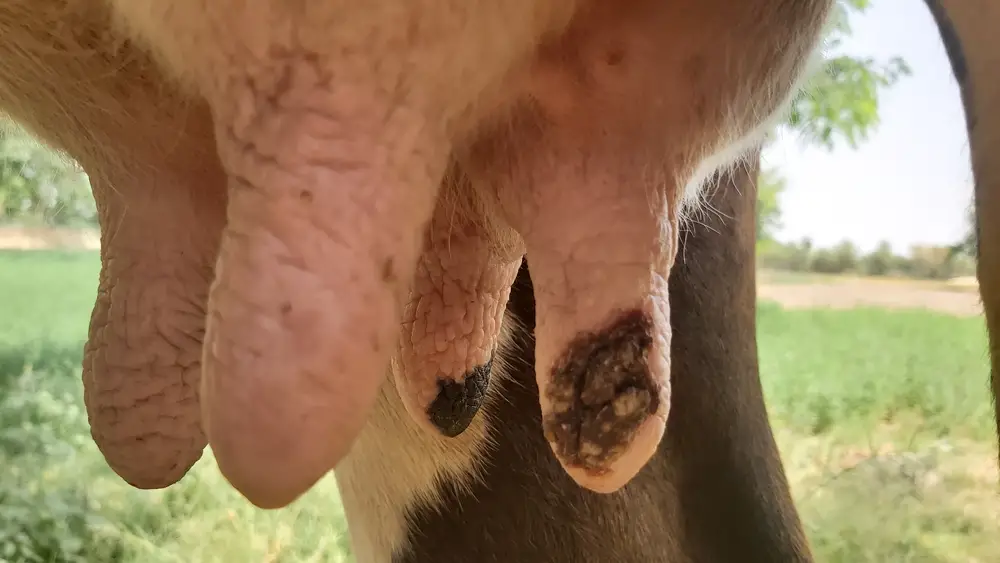
In clinical cases of mastitis, physical signs of mastitis are clearly observable and include udders that are swollen, hot, hard to the touch, and may turn red. When the udder or teats are touched, the cow may kick because this condition is painful.
Milk from a cow with a clinical case of mastitis may appear watery with flecks and clots throughout. It may have a reddish tinge from blood or contain pus as the cow’s immune system struggles to fight the infection.
Milk yields will be drastically reduced when cows have a clinical case of mastitis. They often will not want to walk and may appear distressed.
Other systemic signs will point to an acute case of mastitis including:
- Food avoidance and anorexia
- High rectal temperature
- Lethargy and decreased motility
- Sunken Eyes
- Diarrhea
Some forms of acute mastitis are so severe that they may cause death within a span of 12 hours without medical attention. That is why it is critical to understand the different types of mastitis and the pathogens that cause it.
Types of Mastitis
There are two main origins that lead to mastitis, and they are rooted in the type of pathogen responsible for the infection. The two types are environmental mastitis and contagious mastitis.
Contagious Mastitis
Contagious mastitis occurs when mastitis pathogens are easily spread between cows.
The milking process offers the infected glands the perfect opportunity to spread to other cows as the infected glands are expressed, releasing the microbes responsible for the infection.
Milking machines that are used on multiple cows are notorious for spreading mastitis through a herd. Transmission also occurs through the hands of people manually milking cows when gloves are not worn and exchanged during milking.
Types of contagious pathogens that may spread through milking are Mycoplasma spp, Staphylococcus aureus, and Streptococcus agalactiae.
Environmental Mastitis
Environmental mastitis is caused by pathogens that live in the environment in which a cow spends its time. Transmission occurs following the milking process as teats that are still leaking come into contact with contaminated surroundings such as soil, water, manure and bedding.
Some common environmental microorganisms causing mastitis are Klebsiella spp, Streptococcus uberis, and Escherichia coli, also known as e.coli. These gram-negative bacteriological pathogens enter the udder tissue through prolonged exposure in a contaminated environment.
Humidity and high heat are precursors to bacterial growth, and cows are more likely to be exposed in warmer weather and in humid climates.
Other Causes of Mastitis
Complicating matters, one of the most commonly diagnosed causes of mastitis stems from neither environmental or contagious pathogens, but rather organisms that come from normal skin flora.
Coagulase negative staphylococci live on the skin of a cow and may invade a mammary gland when given the opportunity to do so, causing infection. CNS are not well understood by researchers and a great deal of debate exists on how to properly classify them.
According to this Canadian study, Staphyloccoci can be divided into two separate groups, based on an ability of proteins to cause clotting when mixed with rabbit plasma. These two groups are coagulase-positive and coagulase-negative.
The study included CNS infections within their scope of classification when determining that coagulase-positive and coagulase-negative infections account for the majority of subclinical cases of mastitis during their testing of secretions from cows with mastitis, a result echoed in subsequent samples tested in other countries.
CNS mirrors a pathogen, and while it may be found environmentally, it can also be found on the surface of a cow’s skin in over twenty different isolates, which prevents it from being classified solely as environmental mastitis.
While mastitis of all types occurs in dairy herds, beef cows are also at risk and are experiencing more cases of mastitis than ever before.
It is vital to understand how these pathogens are infecting both types of cows to find the best preventative method to keep herds healthy.
Dairy Cows vs Beef Cows
Both dairy cows and beef cows experience mastitis, yet the causes and frequency differ for both.
Beef Cows
The primary cause of mastitis in beef cows is environmental pathogens.
Beef cows are more likely to get mastitis now than in the past because breeders have been selecting for high milk production in beef cattle, and this leads to cows that have more milk than a calf needs, which makes mastitis more likely.
Common causes of mastitis in beef cows include:
- Teats dirty from manure or mud
- Teat canals still open (leaking milk) when a cow lays down
- Full udders during weaning – cows can injure themselves trying to get to their calves
- Greater prevalence in high-producing, older cows with long, distended udders
- Rain creates an environment where pathogens can enter bedding, or mud and manure
- Teats become injured from sunburn or frostbite, which leads to cows not allowing calves to nurse
Beef cows usually have subclinical cases with little outward signs and usually get better on their own though milk production will be noticeably less.
Dairy Cows
The primary cause of mastitis in dairy cows is contagious pathogens.
Dairy cows have far more mastitis than beef cows, primarily because their udders are regularly used for milking and their teats are open for longer which allows for more exposure.
Common causes of mastitis in dairy cows include:
- The teat orifice takes 2 hours to close completely following milking and it is during this time that it is open to infection
- Pathogens enter the teats frequently through the use of milking machines
- Contaminated hands can cause the spread of contagious pathogens through manual milking of multiple cows
- Contagious pathogens can be spread by insects such as flies
- A calf may also infect her mother through suckling by the transmission of contaminants that are in the calf’s mouth.
Farms that have dairy cows are more vigilant in looking for signs of mastitis and focusing on prevention to reduce cases in their herds.
Prevention
Milking Practices
Management of the milking routine and equipment is vital in limiting mastitis risk. Milking machine systems must be regularly maintained and cleaned to ensure no cross-contamination occurs between cows.
It is vital to ensure cows are not over-milked because this causes damage to the teat which increases mastitis risk. Likewise, if cows are not sufficiently milked, this can decrease milk production and lead to mastitis.
Vaccination
Vaccines can be an important tool in mastitis control.
One example is the J5 core antigen vaccine which has been used since the 1990s and has proven effective in lowering the incidence of E. coli in clinical cases of mastitis.
Vaccines are still being created to fight mastitis because few of them are effective for coliform infections. It is important to continue to stay on top of new vaccines for cows for preventative purposes.
Mycotoxin Management
Limiting mycotoxin exposure is important for the overall health of cows, in addition to limiting mastitis risk. High-stress increases mycotoxins so it is vital to handle herds with care, especially during calving and lactation.
Mycotoxins can be found in feed and are known to suppress the immune system leading to cows eating less, and being predisposed to diseases and metabolic disorders.
Mycotoxins lead to reduced milk production and can cause nutrient absorption issues, which impairs milk synthesis so it is important to minimize mycotoxins.
It is recommended that feed is regularly tested for mycotoxins, and the use of toxin binders should be added to feed to counteract the effects of mycotoxins.
Hygiene
Proper hygiene is of paramount importance in the barn and in the parlor. Surfaces should be regularly cleaned and cattle-specific bedding should be used.
Clean sand is widely considered the best bedding for cows as the material doesn’t allow for the growth of microorganisms.
Nutrition
Nutrition is a major factor in preventing mastitis. Cows that have a negative energy balance are more likely to have health issues and infections.
Transition cows in particular are at high risk for nutritional deficits. A proper diet must be maintained including minerals and vitamins for the immune system to function optimally.
Weather
The weather unfortunately cannot be controlled, but understanding the correlation between weather and mastitis is important.
Excessive rain can lead to contaminated water and mud, which cows may lay in with exposed teats. Likewise, heat and humidity cause pathogen populations to grow quickly.
During extreme weather events, it is important to do everything possible to keep a clean environment to minimize exposure keeping udder health in mind.
Flooring
Proper flooring that leads into the parlor and barn areas should be solid, and free from debris that may unintentionally cause injury to a cow’s udder.
It is important to keep the milking process as stress-free as possible, with the aim of injury prevention as damaged tissue can allow for bacteria to infect the mammary glands.
Feed Timing
It is important to ensure that new feed is taken to the cow pen while cows are in the parlor.
This will help them want to remain to stand and eat rather than laying down when their teats are still open. It ultimately reduces how often cows are exposed to pathogens which can lead to mastitis.
Diagnostic Testing and Record Keeping
It is vital to test cows that appear to have mastitis. Taking a milk sample and submitting it for testing is recommended by veterinary medicine experts.
Recording the results of tests is important to identify trends within individual beef and dairy farms, as well as wider trends within the dairy industry.
There are several different types of tests for mastitis. The first test will be to determine if mastitis is present.

The California Mastitis Test can clearly show mastitis. It can be performed by farmers at home and doesn’t require the use of a lab. This test measures leucocytes through viscosity and is great for showing the severity of mastitis present.
Another test often used for determining if mastitis is present requires sending a sample to a lab and is called the SCC test. This test measures the amount of SCC’s in a milliliter of milk.
SCC stands for somatic cell counts and the test examines the number of white blood cells present.
- SCC’s signaling infection can be as little as 100k cells per ml.
- SCCs that have greater than 280k per ml have around an 85 percent infection chance.
It should be noted the SCC test and the California Mastitis Test do not tell you what is causing the mastitis. For that information, you will need another test.
There are a few different options that will show you the cause of the infection.
A sample of milk can be sent to a lab to perform a bacterial culture from the area(s) that show signs of infection. While this is a reliable way of determining the cause, it can take one to two weeks to get results which may be too long.
Another test is the ELISA test, which will show the type of pathogen but will not let you know if mastitis is present.
The Multiplex PCR test is the gold standard capable of identifying mastitis, the pathogen behind it, and is both reliable and fast. This type of test also allows for fresh, preserved, or frozen milk testing.
Treatment
Once mastitis has been identified in a cow, ice should be used on the surface of the udder to reduce swelling and pain.
Infested teats will require draining three times a day, and all of the milk should be properly disposed of to prevent the spread of infection. Adding 5 percent phenol to the milk that is discarded will ensure it is safe to throw out.
When draining the teats of infected cows, ensure that the healthy cows have already been milked to reduce cross-contamination. Handling infected teats requires the utmost respect for hygiene and cleanliness as residues can contain harmful pathogens.
Dry Cow Therapy
One of the most important treatment methods for farmers in fighting mastitis is dry cow therapy. This takes advantage of the dry period that cows have between lactation periods when they can have antibiotic treatment.
The drying-off period is a beneficial time to treat mastitis as milk loss is greatly reduced. However, environmental pathogens are more likely to cause infection right at the end of lactation, and again at the end of the dry period during calving.
Cows that are at the end of the lactation period can be treated with antimicrobial teat dip which is best-used post-milking and germicidal teat dip prior to milking which reduces the incidence of environmental pathogen infection.
Pain Management
Acute mastitis can be treated with NSAID medications such as ibuprofen, flurbiprofen, carprofen, and ketoprofen for pain management and reduction of swelling. Always consult a veterinarian before administering these or any other medications to get the appropriate dosage.
Culling
While never a first resort, culling cows that have chronic or untreatable mastitis can prove a necessity to keep it from spreading through the healthy heifers and cows in the herd.
Culling should only be necessary in the most extreme cases.
FAQs
How Does Mastitis Affect a Cow’s Milk?
Reduction of milk quality and milk quantity occurs in mastitic cows, mainly from the increase of somatic cell counts which naturally increase to fight invading pathogens in the mammary gland.
Mastitis changes the amounts of milk components present within milk such as lactose, protein, fat, and mineral content. Mastitis may cause more sodium and less potassium to be present in milk.
Milk from cows with mastitis may contain pus or blood and have chunks or flecks in it. There will be an increasing amount of visual evidence of infection depending on how severe the infection is.
Dairy farmers should discard milk from infected cows.
What is Toxic Mastitis?
Toxic mastitis is a particularly severe form of mastitis which causes inflammation far more acute than regular cases. It can even cause septicemia which is deadly to cows within hours If not immediately treated.
According to Farm Health Online, “The signs are primarily due to the endotoxin produced by the bacteria, causing the cow to develop endotoxic (also known as toxaemic) shock. The cow will present as acutely sick, dull, and may be recumbent. She may have a high temperature or conversely may have a sub-normal temperature if in shock.”
If cows present with these symptoms, a veterinarian is needed immediately to test and administer treatment.
What is Chronic Mastitis?
Chronic mastitis is mastitis that never fully disappears, either from not being treated properly or the conditions causing the infection are still present and continue to cause re-infection.
The most common cause of chronic mastitis is a shed or barn not being properly cleaned.
Once mastitis reaches the chronic stage, hard lumps will form in the udder, and fibrosis may occur. Once fibrosis sets in, treatment is unlikely to be effective and cows must be culled from the herd to prevent infection of healthy animals.
How Long Does Mastitis Last in Cows?
Mastitis can be short-lived if immediately treated with the help of a veterinarian. It can clear up following a round of antibiotics (if from a bacterial infection) and may only take a few days to a few weeks.
Unfortunately, viral causes can take longer to cure. Mastitis that has been allowed to remain untreated is likely to persist if it reaches a clinical case.
Ensure mastitic cows are given enough antibiotics over a proper duration to see if they improve.
Unfortunately, not every cow will respond to treatment even if treated properly. In that event, it may be necessary for the culling of an unresponsive cow to save the rest of the herd.
